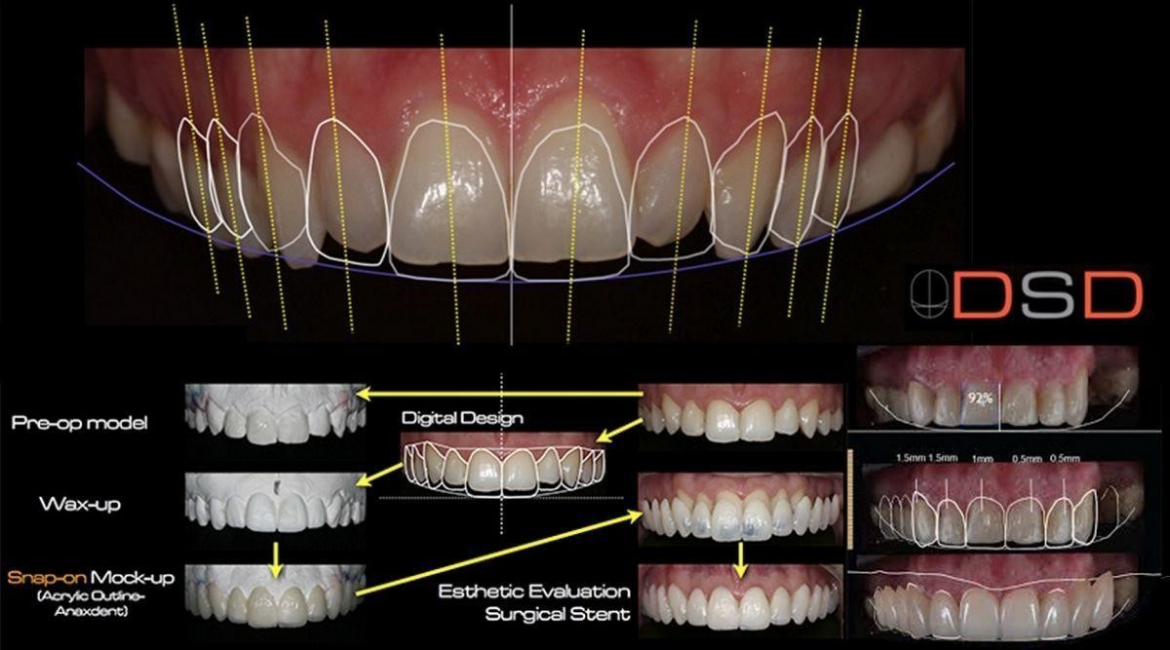
To obtain consistent esthetic outcomes, the design of dental restorations should be defined as soon as possible. The importance of gathering diagnostic data from questionnaires and checklists cannot be overlooked; however, much of this information may be lost if it is not transferred adequately to the design of the restorations. The diagnostic data must guide the subsequent treatment phases, integrating all of the patient’s needs, desires, and functional and biologic issues into an esthetic treatment design.
The Digital Smile Design (DSD) is a multi-use conceptual tool that can strengthen diagnostic vision, improve communication, and enhance predictability throughout treatment. The DSD allows for careful analysis of the patient’s facial and dental characteristics along with any critical factors that may have been overlooked during clinical, photographic, or diagnostic cast–based evaluation procedures. The drawing of reference lines and shapes over extra- and intraoral digital photographs in a predetermined sequence can widen diagnostic visualization and help the restorative team evaluate the limitations and risk factors of a given case, including asymmetries, disharmonies, and violations of esthetic principles.1 DSD sketches can be performed in presentation software such as Keynote (iWork, Apple, Cupertino, California, USA) or Microsoft PowerPoint (Microsoft Office, Microsoft, Redmond, Washington, USA). This improved visualization makes it easier to select the ideal restorative technique.
The DSD protocol is characterized by effective communication between the interdisciplinary dental team, including the dental technician. Team members can identify and highlight discrepancies in soft or hard tissue morphology and discuss the best available solutions using the amplified images. Every team member can add information directly on the slides in writing or using voice-over, thus simplifying the process even more. All team members can access this information whenever necessary to review, alter, or add elements during the diagnostic and treatment phases.
The adoption of the DSD protocol can make diagnosis more effective and treatment planning more consistent. The efforts required to implement DSD are rewarded by more logical and straightforward treatment sequencing, leading to savings in time, materials, and cost during treatment.
Table of Contents
Digital Smile Design
The DSD protocol offers advantages in the following areas:
• Esthetic diagnosis
• Communication
• Feedback
• Patient management
• Education
Esthetic Diagnosis
When the dentist first evaluates a new patient with esthetic concerns, many critical factors may be overlooked. A digital photography and digital analysis protocol enables the dentist to visualize and analyze issues that he or she may not notice clinically. Drawing of reference lines and shapes over extra- and intraoral digital photographs can easily be performed using
presentation software.
Communication
Traditionally, smile design has been instituted by the dental technician. The technician performs the restorative wax-up, creates the tooth shapes and dental arrangements, and follows the instructions and guidelines provided by the dentist in writing or by phone. In many cases, however, insufficient information is given to the dental technician to utilize his or her skills to maximum potential. As a result, the final restoration is less likely to fully satisfy the patient’s desires.
When the treatment coordinator or whichever member of the restorative team has developed a personal relationship with the patient takes responsibility for the smile design, the results are likely to be far superior.
This individual has the ability to better communicate the patient’s personal preferences and/or morphopsychologic features to the technician, elevating the excellence of the restoration from acceptable to exceptional.
Successful restorative treatment involves controlling the four dimensions of treatment: esthetics, function, structure, and biology. In relation to esthetics, there are four main issues that must be controlled to improve predictability and meet patient expectations: the horizontal reference plane, facial midline, smile design (tooth shape and arrangement), and color. The question is how to precisely transfer this information from the face to the mouth, to the cast, and to the final restoration. The primary goal of the DSD protocol is to facilitate this process.
With this valuable information in hand, the dental technician can more efficiently fabricate a three-dimensional wax-up, focusing on developing anatomical features within the parameters provided, including the planes of reference, facial and dental midlines, recommended incisal edge position, lip dynamics, basic tooth arrangement, and incisal plane.
This information is transferred from the wax-up to the try-in phase through a mock-up or provisional restoration. The design of the definitive esthetic restorations should be developed and tried-in as soon as possible to guide the treatment sequence. Efficient treatment planning helps the entire dental team identify any challenges and reduce total treatment time.
Feedback
The DSD allows for precise evaluation of the results obtained in every treatment phase. The sequence of treatment is organized on the slides with photographs, videos, notes, graphics, and drawings. At any time, team members can access the slide presentation to
track and analyze the treatment provided. With the digital ruler, drawings, and reference lines, easy comparisons can be made between pre- and posttreatment photographs. These comparisons help determine whether the treatment has successfully followed the original plan or if other adjunctive procedures are necessary to improve the final outcome. The dental technician also gains feedback related to tooth shape, arrangement, and color to facilitate any necessary refinements. This constant double-checking ensures the excellence of the final result and provides a great learning tool for the entire interdisciplinary team. The DSD tool also serves as a useful library of treatment procedures. Clinicians can revisit treatments performed years ago and learn from past results.
Patient Management
The DSD can be used as a marketing tool to motivate the patient, an educational tool to help explain issues related to treatment, and an evaluative tool by comparing before and after photographs. Further, the library of slides from past treatments can be used to demonstrate treatment possibilities during patient consultation. The treatment planning presentation will be much more effective because the DSD allows patients to visualize the multiple factors responsible for their orofacial issues. The problems presented in each case can be superimposed in list form directly over the patient’s own photographs. The clinician can express the severity of the case, introduce treatment strategies, discuss the prognosis, and make case management recommendations. In addition, DSD aids in patient acceptance by helping them visualize and understand both past and future treatments.
Education
This personal library of clinical cases can also be shared with patients and colleagues, and the most appropriate cases can be transformed into a slideshow for dental presentations and lectures. DSD can increase the visual impact of a lecture by incorporating the slides from clinical cases. The audience can better understand the concepts discussed, and the presenter can minimize the use of a laser pointer.
DSD Workflow
The authors carry out the DSD protocol using Keynote software (iWork); however, similar software such as Microsoft PowerPoint can be used with minor adjustments to the technique. Keynote allows for simple manipulation of the digital images and the addition of lines, shapes, and measurements over the clinical and
laboratory images.
 Three basic photographic views are necessary: full face with a wide smile and the teeth apart, full face at rest, and retracted view of the full maxillary arch with teeth apart. A short video is also recommended in which the patient is prompted by the clinician to explain his or her treatment concerns and expectations. Simultaneously, the video should capture all possible dental and smile positions, including 45-degree and profile views. The photographs and videos are downloaded and inserted into the slide presentation. The DSD workflow then proceeds as follows:
Three basic photographic views are necessary: full face with a wide smile and the teeth apart, full face at rest, and retracted view of the full maxillary arch with teeth apart. A short video is also recommended in which the patient is prompted by the clinician to explain his or her treatment concerns and expectations. Simultaneously, the video should capture all possible dental and smile positions, including 45-degree and profile views. The photographs and videos are downloaded and inserted into the slide presentation. The DSD workflow then proceeds as follows:
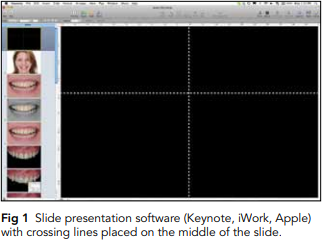
1. The cross: Two lines must be placed on the center of the slide, forming a cross (Fig 1). The facial photograph with the teeth apart should be positioned behind these lines.
2. Digital facebow: Relating the full-face smile image to the horizontal reference line is the most important step in the smile design process. The interpupillary line should be the first reference line to establish the horizontal plane, but it should not be the only one. The face as a whole must be analyzed before determining the best horizontal reference to achieve harmony. After determining the horizontal reference line, the facial midline is outlined according to facial features such as the glabella, nose, and chin (Fig 2).
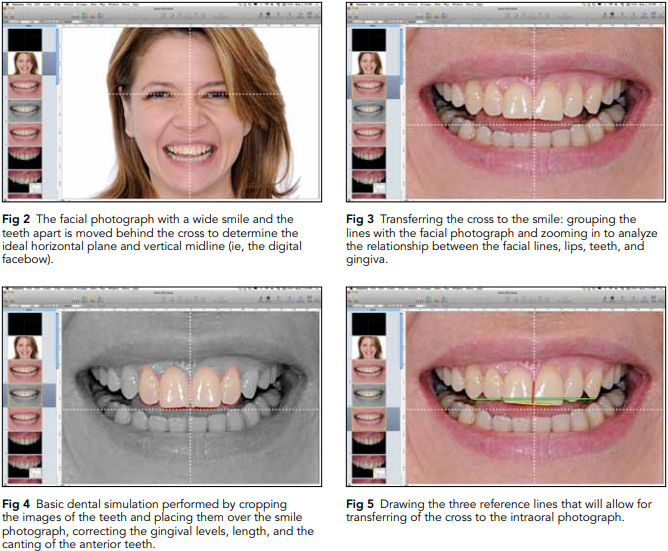 3. Smile analysis: Dragging the horizontal line over the mouth will allow for initial evaluation of the relationship of the facial lines with the smile. Grouping the lines and the facial photographs will allow the clinician to zoom in on the image without loosing the reference between the lines and photograph. Midline and occlusal plane shifting and canting can be easily detected (Fig 3).
3. Smile analysis: Dragging the horizontal line over the mouth will allow for initial evaluation of the relationship of the facial lines with the smile. Grouping the lines and the facial photographs will allow the clinician to zoom in on the image without loosing the reference between the lines and photograph. Midline and occlusal plane shifting and canting can be easily detected (Fig 3).
4. Smile simulation: Simulations can be performed to fix the incisal edge position, canting, shifting, tooth proportions, and soft tissue outline (Fig 4).
5. Transferring the cross to the intraoral images: To analyze the intraoral photographs in accordance with the facial references, the cross must be transferred to the retracted view using three transferring lines drawn over the smile view as follows (Fig 5):
a) Line 1: from the tip of one canine to the tip of the contralateral canine.
b) Line 2: from the middle of the incisal edge of one central incisor to the middle of the incisal edge of the contralateral central incisor.
c) Line 3: over the dental midline, from the tip of the midline interdental papillae to the incisal embrasure.
It is necessary to calibrate four features on the photograph: size, canting, incisal edge position, and midline position. Line 1 will guide the two first aspects (size and canting), line 2 will guide the incisal edge position, and line 3 will guide the midline position (Fig 6).
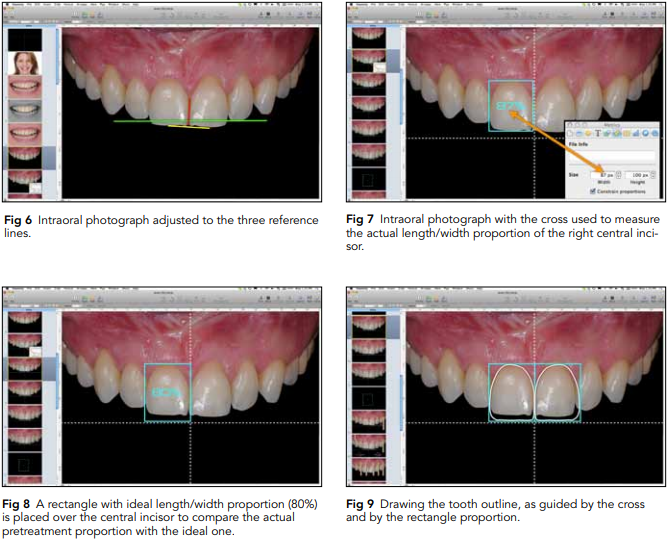 6. Measuring tooth proportion: Measuring the width/ length proportion of the central incisors is the first step toward understanding how to best redesign the smile. A rectangle is then placed over the edges of both central incisors (Fig 7). The proportions of the patient’s central incisors can be compared to the ideal proportions described in the literature (Fig 8).
6. Measuring tooth proportion: Measuring the width/ length proportion of the central incisors is the first step toward understanding how to best redesign the smile. A rectangle is then placed over the edges of both central incisors (Fig 7). The proportions of the patient’s central incisors can be compared to the ideal proportions described in the literature (Fig 8).
7. Tooth outline: From this step on, all drawings may
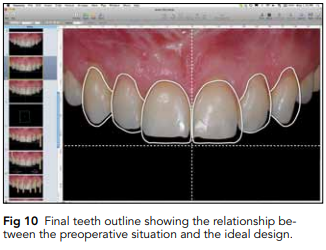
be performed depending on what needs to be visualized or communicated for each specific case. For example, tooth outlines can be drawn over the photograph, or premade tooth outlines can be copied and pasted. The selection of tooth shape will depend on factors such as the morphopsychologic interview and the patient’s desires, facial features, and esthetic expectations (Figs 9 and 10).
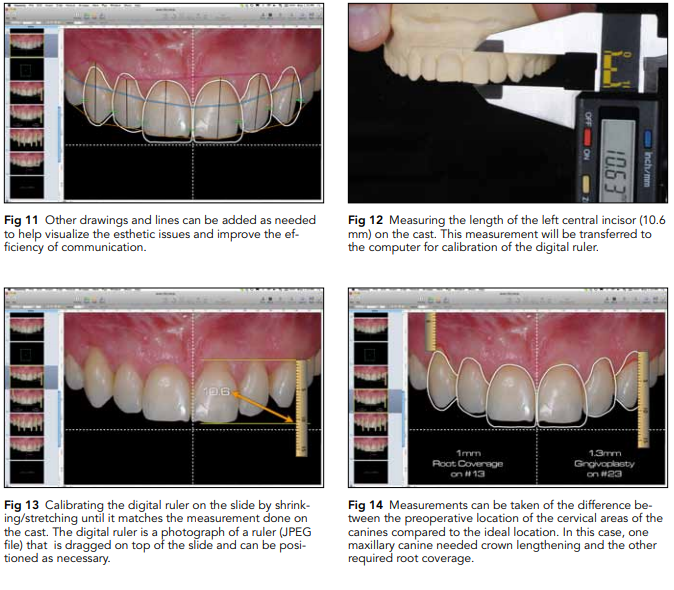 8. White and pink esthetic evaluation: After all reference lines and drawings have been provided, the clinician should have a clear understanding of the esthetic issues involved in the patient’s maxillary arch, including the tooth proportions, interdental relationship, relationship between the teeth and smile line, discrepancy between facial and dental midlines, midline and occlusal plane canting, soft tissue disharmony, relationship between the soft tissues and teeth, papillae heights, gingival margin levels, incisal edge design, and tooth axis (Fig 11).
8. White and pink esthetic evaluation: After all reference lines and drawings have been provided, the clinician should have a clear understanding of the esthetic issues involved in the patient’s maxillary arch, including the tooth proportions, interdental relationship, relationship between the teeth and smile line, discrepancy between facial and dental midlines, midline and occlusal plane canting, soft tissue disharmony, relationship between the soft tissues and teeth, papillae heights, gingival margin levels, incisal edge design, and tooth axis (Fig 11).
9. Digital ruler calibration: The digital ruler can be calibrated over the intraoral photograph by measuring the length of one of the central incisors on the cast (Fig 12) and transferring this measurement to the computer (Fig 13). Once the digital ruler
is calibrated, the clinician can make any measurements needed over the anterior area of the image (Fig 14).
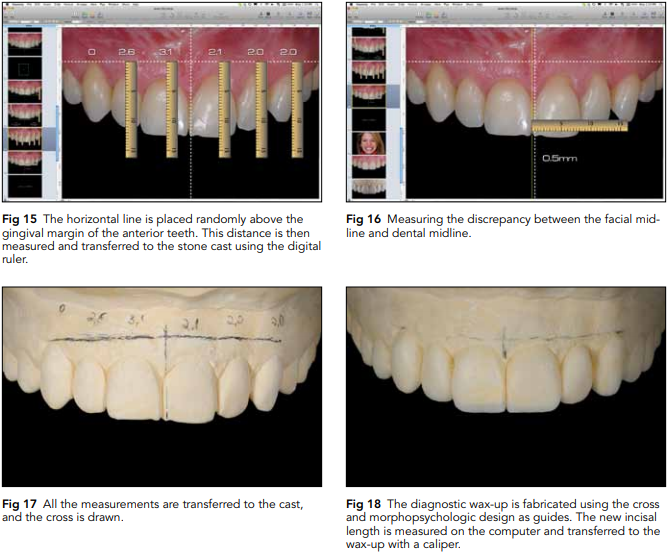
10. Transferring the cross to the cast: First, the horizontal line over the intraoral photograph should be moved above the gingival margin of the six anterior teeth. The distance between the horizontal line and the gingival margin of each tooth is measured using the digital ruler, and these measurements are written down on the slide (Fig 15). The measurements are then transferred to the cast with the aid of a caliper. Pencil marks are made on
the cast at the same distances above the gingival margins as shown on the digital images. Those dots are then connected, creating a horizontal line above the teeth. The next step is to transfer the vertical midline. Because the vertical line must be perpendicular to the horizontal line, only one point is necessary to determine its location. The distance between the dental midline and the facial midline at the incisal edge is measured on the computer, and the distance is then transferred to the cast with the caliper (Fig 16). Subsequently, the line can be drawn perpendicular to the horizontal line passing over this reference point. After drawing the cross on the cast (Fig 17), it is possible to transfer any necessary information, such as gingival margins, root coverage, crown lengthening, incisal edge reduction, and tooth width. At this stage, all information the technician will need to develop a precise wax-up is available on both the slides and cast (Fig 18).
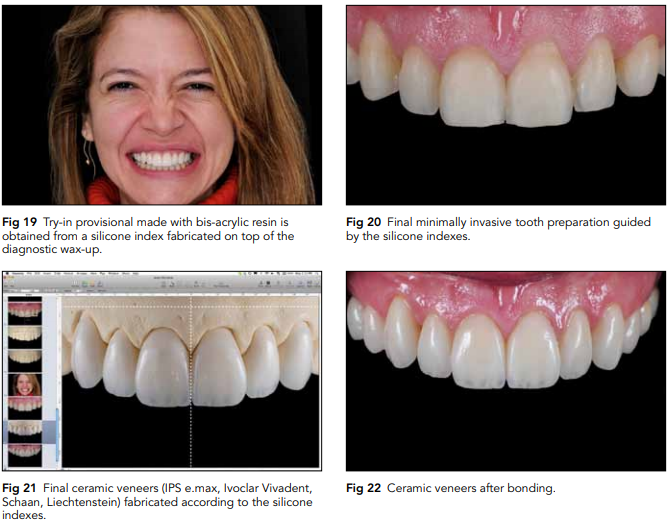
 The guided diagnostic wax-up will be an important reference for any surgical, orthodontic, and restorative procedures. Several guides can be produced over this wax-up to control the procedures, such as surgical stents, orthodontic guides, implant guides, crown lengthening guides, and tooth preparation guides. The next important step to evaluate the precision of the DSD protocol and the wax-up is to perform a clinical try-in (Fig 19). The clinical try-in can be carried out using a direct mock-up or a provisional restoration depending on the complexity of the case. After patient approval, the restorative procedures can be adjusted as necessary. Tooth preparation should be minimally invasive, allowing just enough clearance to create proper space for ceramic restorations (Fig 20). Fabrication of the final restorations should be a controlled process with minimal final adjustments (Fig 21). If all of
The guided diagnostic wax-up will be an important reference for any surgical, orthodontic, and restorative procedures. Several guides can be produced over this wax-up to control the procedures, such as surgical stents, orthodontic guides, implant guides, crown lengthening guides, and tooth preparation guides. The next important step to evaluate the precision of the DSD protocol and the wax-up is to perform a clinical try-in (Fig 19). The clinical try-in can be carried out using a direct mock-up or a provisional restoration depending on the complexity of the case. After patient approval, the restorative procedures can be adjusted as necessary. Tooth preparation should be minimally invasive, allowing just enough clearance to create proper space for ceramic restorations (Fig 20). Fabrication of the final restorations should be a controlled process with minimal final adjustments (Fig 21). If all of
these steps are carried out properly and carefully, the final result will likely exceed the patient’s expectations (Figs 22 and 23).
 Conclusions
Conclusions
The Digital Smile Design is a multi-use tool that can assist the restorative team throughout treatment, improving the dental team’s understanding of the esthetic issues and increasing patient acceptance of the final result. The placement of references lines and other shapes over extra- and intraoral digital photographs widens the dental team’s diagnostic vision and helps to evaluate the limitations, risk factors, and esthetic principles of a given case. These critical data will lead to improved results in all phases of treatment.